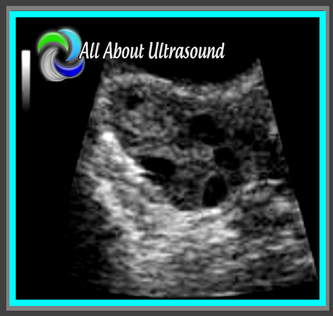
 2. Scanning and trying to find those ovaries can prove to be a challenge with a pregnant uterus! Even though it is not our focus, we can’t forget those ovaries! Making sure to image those along with the uterus and fetal images will ensure that you’re not missing potential pathology, but it can definitely be tough with that pregnant uterus in the way. Best methods are to bring the transducer laterally to the patient’s side and to scan in a transverse plane along the lateral side of the uterus, starting pretty high up and moving down toward the patient’s cervix. That transverse plane will give you an increased field of view and will allow you to identify structures more easily.
16 Comments
Marisa Morris
7/21/2017 06:38:24 am
Reply
Kathy Brewer
7/21/2017 07:24:03 pm
Reply
Marlon Rimando
7/22/2017 07:29:31 am
Nice topic!
Reply
dr rahella
9/5/2017 12:25:16 pm
show
Reply
3/13/2018 06:12:30 pm
My wife and I finally got pregnant and we couldn't be more excited for our family to grow. I really appreciate you helping identify some things in the ultrasound with these pictures. We will look for these things in our pictures.
Reply
6/5/2018 11:49:30 pm
This is some really good information about gynecologist. It is good to know that it would be smart to have a scan done because it can help you position the baby well. That does seem like a good thing to know that because my sister just got pregnant.
Reply
7/2/2018 05:37:55 am
Great Blog and thanks for sharing such informative blog. It will definitely help everyone with this information.
Reply
6/22/2020 10:26:54 pm
We just found out that my sister is pregnant through PT; that's why we're currently looking for an Obstetrics for her. Since I am not an expert in this, I never knew that the doctors must scan with color Doppler flow, so they'll be able to locate the umbilical cord. It's also interesting to learn that aorta will still arch around, even if it already left the heart.
Reply
11/7/2020 11:05:09 am
You have covered each points very precisely. The post couldn't be any better.
Reply
I love that you pointed out that it could be very exciting to find the gender of our little ones through ultrasound. I can't wait for that day when we are able to see our child through that procedure. Hopefully, we will be able to conceive this year because my husband and I have finally decided to start having babies this year.
Reply
2/9/2022 09:29:43 pm
I didn't know that the sound in ultrasounds were outflow tracks. My wife needs an ultrasound. She thinks that she is pregnant.
Reply
8/16/2022 07:54:36 pm
It's interesting when you said that potential pathology should be seen throughout the scanning of the baby. As we moved to our current area, my spouse told me about the importance of choosing a gynecologist for her proper prenatal care. I appreciate this instructive article, I'll tell her that I'll do some research and ask for referrals to find a reputable gynecologist for more information.
Reply
8/30/2022 12:52:58 am
Wow, it's amazing to know that a lot of a baby's vitals can be measured through ultrasound. I'm interested in looking for an OBGYN clinic soon because I recently experience my baby kicking from inside me for the first time. I might need to look more into that before I give birth.
Reply
Leave a Reply. |
Details
Making Waves™All About Ultrasound presents Making Waves™, our ultrasound specific blog and newsletter. Join us here for ultrasound news, cases and more! Don't FORGET YOUR MERCH!Archives
May 2023
Categories
All
|

 RSS Feed
RSS Feed